Skin Care Tips for a Radiant Complexion
- posted: Aug. 14, 2023
- Skin Care
Taking care of your skin is important. Your skin is the largest organ in your body and it’s crucial that you’re giving it all the nourishment that it needs. Learning Read More
The Power of Chemical Peels
- posted: Aug. 01, 2023
- Skin Treatments
When you have healthy skin, with an even skin tone, you just naturally look better. You look younger and more vibrant. Unfortunately, aging, sun exposure, environmental toxins, and other factors Read More
Understanding Acne: Causes and Treatment Options
- posted: Jul. 13, 2023
- Skin Care
Acne is an extremely common condition that people around the country struggle with. Acne is often associated with puberty and teenagers, but it can affect you at any age. Acne Read More
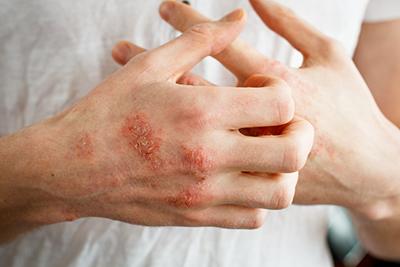
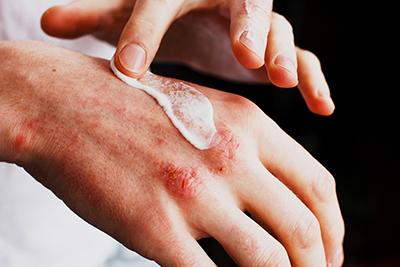
Treating Eczema in Adults
- posted: Jul. 01, 2023
- Skin Conditions
Eczema, also known as atopic dermatitis, is a chronic skin condition characterized by red, itchy, and inflamed patches on the skin. It affects millions of people worldwide, both children and Read More
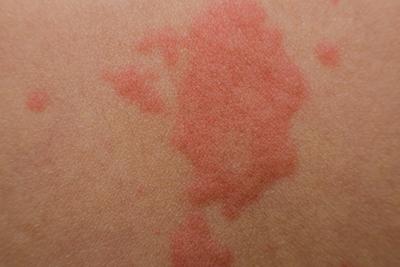
Common Causes of Rashes
- posted: Jun. 22, 2023
- Skin Conditions
Your dermatologist treats a wide variety of skin rashes. When you have an uncomfortable, itchy, irritated skin rash, it’s nice to know you can get help from an expert-your dermatologist. What Read More
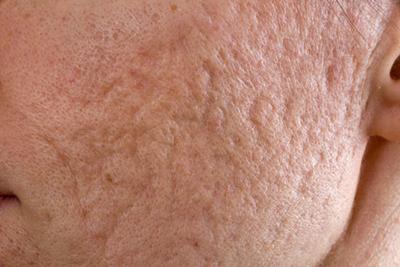
Treatment Options for Acne Scarring
- posted: Jun. 06, 2023
- Skin Care
Acne is a common problem, and it’s a problem that may continue with acne scarring. If you have acne scarring, you will be happy to know that your dermatologist can Read More
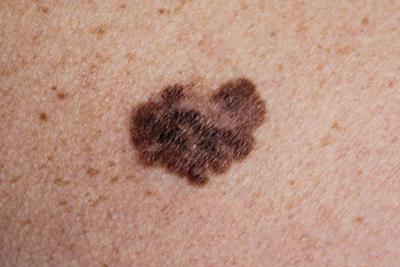
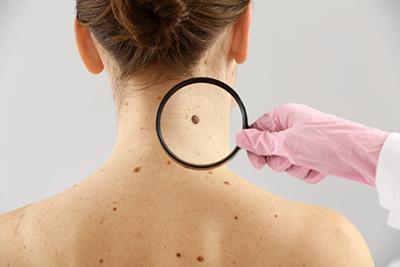
The ABCDEs of Skin Cancer: Understanding the Signs and Symptoms
- posted: May 16, 2023
- Skin Conditions
When it comes to your skin, it’s important that you’re taking precautions to keep it safe, healthy, and protected from issues like skin cancer. With skin cancer, the most important Read More
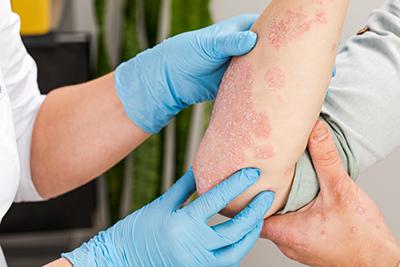
Eczema: Understanding Triggers and Treatment Options
- posted: May 08, 2023
- Skin Conditions
Eczema is a skin condition that can leave you feeling itchy and dry. Dealing with eczema can be annoying and you might find that a flare-up can be irritating and Read More
Common Skin Conditions: Eczema, Psoriasis, and Rosacea Explained
- posted: Apr. 21, 2023
- Skin Conditions
The skin is sensitive and there are many conditions that could affect your skin. There are a few that have similar symptoms and they even tend to look similar. Three Read More
Skin Cancer Prevention Tips
- posted: Apr. 07, 2023
- Skin Care, Dermatology
It feels great to be out in the sun. Unfortunately, while you are enjoying yourself, the sun is damaging your skin. Excessive sun exposure can lead to skin cancer. There Read More
Skincare Tips for Every Skin Type: How to Keep Your Skin Healthy and Radiant
- posted: Mar. 23, 2023
- Skin Care, Dermatology
When your skin looks dull and drab, you might feel the same way. Dealing with issues like dry or oily skin can be irritating and you may not know how Read More
Understanding Common Skin Conditions and How to Manage Them
- posted: Mar. 10, 2023
- Skin Care, Dermatology, Skin Conditions
There are many skin disorders that people struggle with, and they vary greatly in symptoms and their severities. Some skin conditions can be temporary, while others are permanent and have Read More
Understanding and Managing Acne
- posted: Feb. 27, 2023
- Skin Care
Everyone deals with acne at some point in life. It’s one of the most common issues that your dermatologist deals with on a daily basis. Acne can be difficult to Read More
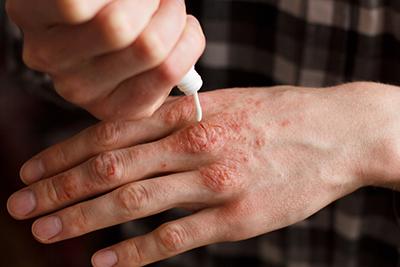
How to Treat and Prevent Eczema Flare-Ups
- posted: Feb. 07, 2023
- Skin Care, Skin Condition, Dermatology, Skin Treatments
If you deal with eczema, you understand that dealing with a flare-up can be irritating and can distract from your normal routine. You might also feel self-conscious about it being Read More
The Benefits of Regular Skin Cancer Screenings
- posted: Jan. 25, 2023
- Skin Care, Dermatology, Skin Treatments
Your dermatologist is an important part of your healthcare team. Your dermatologist performs a vital service that could save your life–regular skin cancer screenings. Skin cancer is one of the Read More
Non-Invasive Anti-Aging Treatments
- posted: Jan. 11, 2023
- Skin Care, Skin Condition, Dermatology, Skin Treatments, Nail Care
There are many factors which can combine to make you look older than you are. Sun exposure, harmful chemicals or cosmetics, bad diet, lack of hydration, and the accumulation of Read More